Public Story
MSF TB Uganda
Kitgum, Uganda.
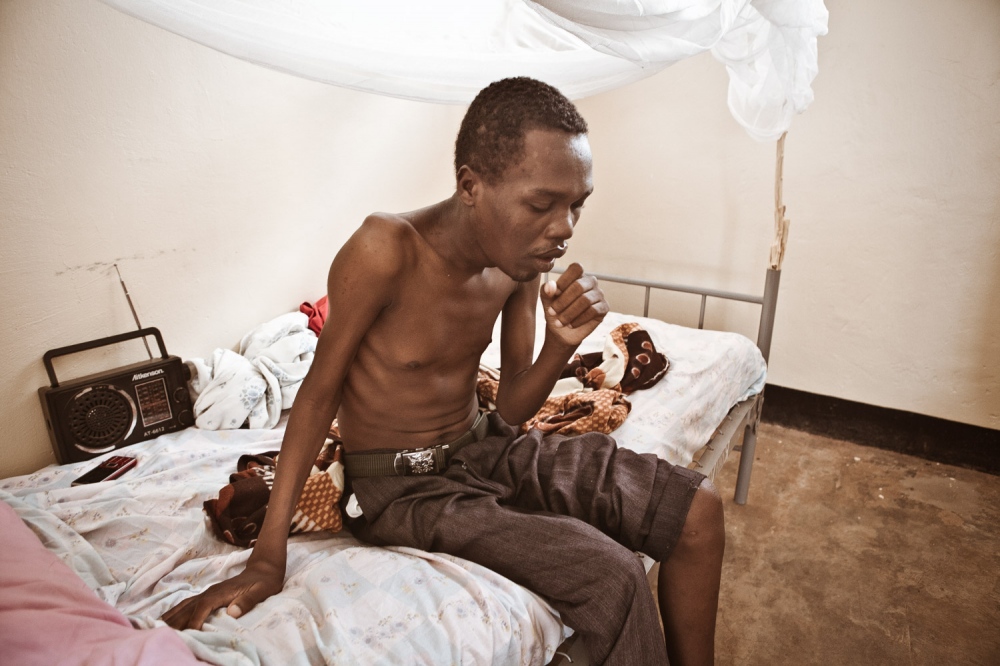
Uganda is one of the world's 22 high burden countries for tuberculosis (TB). MSF's experience of treating drug-resistant tuberculosis (DR-TB) in Uganda strongly suggests that centralised care is not the answer. Many patients and their caregivers from rural districts will find it impossible to manage a lengthy stay in the capital, and default rates are likely to skyrocket. Since 2009, MSF has been running a community-based and comprehensive TB treatment programme in Kitgum, in northern Uganda, hand in hand with the Ministry of Health.
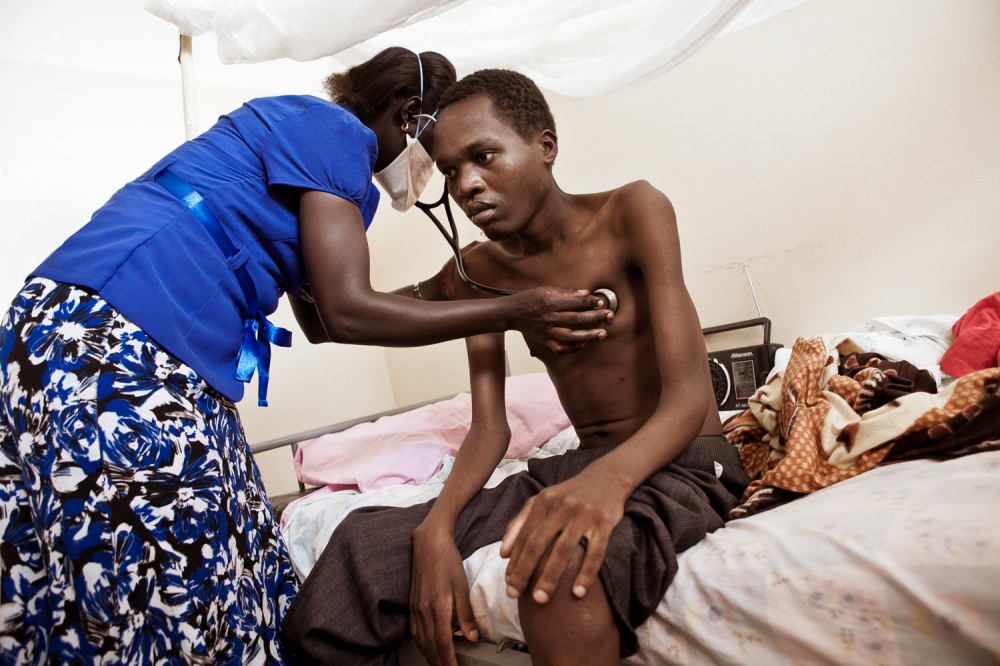
tMSF puts the success down to the model of care they are using, which is comprehensive, decentralised, and community-based. In addition to the conventional components of care, three constituents have played a vital part: the home-based care approach, food incentives, and and the use of village health teams, who are trained, supervised and rewarded for their work. In addition, MSF underscores the need for psychosocial counseling to support patients throughout their treatment.
Community-based care has been shown to be safe, practical and extremely effective for DR-TB, leading to high adherence, close follow-up and encouraging outcomes. Patients treated within their communities benefit from the practical and emotional support of friends and family in coping with the side effects of the drugs and adhering to their treatment, while increased understanding of TB within communities leads to higher detection rates and reduced stigma associated with the disease. The model of care has proved to be feasible and widely accepted "“ by patients, local communities and healthcare staff alike.